It’s not who you think
Authors: Christian González-Rivera, Director of Strategic Policy Initiatives and Ruth Finkelstein, Executive Director, Brookdale Center for Healthy Aging, Hunter College, CUNY
After enduring months of unemployment or adapting to work from home, most people are wondering when and how the economy will open up again. Evidence on the natural history of the novel coronavirus casts doubt on the folk wisdom that herd immunity will eventually make it safe to go to work. A widely accepted, effective vaccine is many months or years away. In the meantime, the possibility of multiple waves of infection sending society into a cycle of lockdowns for the foreseeable future is making the possibility of going back to a “normal” life seem ever so dim.
One message that has remained consistent throughout the public health crisis has been that older adults are at greater risk of getting seriously ill or dying of COVID-19. This has prompted some economists and policymakers to suggest that most people could return to work if we maintain a lockdown for people aged 65 and older and open the economy for everyone else.
Simply put, such a plan is not only terribly immoral and unjust, but it will also fail to accomplish its two main objectives: to restart the economy and to contain the virus. Instead, extended isolation will exact a terrible cost on the physical, mental, and emotional well-being of older Americans.
A plan to isolate older adults fails to look deeper into the COVID-19 data to find important patterns other than age that are driving the pandemic’s death toll. When the fatality data is disaggregated by age, presence of underlying conditions, and being a resident of a long-term care facility, a much more nuanced picture of who is at risk emerges. This level of nuance is critically important to making informed decisions about how to reopen the economy as safely as possible.
In this article, we present an analysis of data from various sources that shows that policymakers are asking the wrong questions when weighing how to safely reopen the economy. They are asking who needs to be protected rather than asking what needs to be done to make all workplaces as safe as possible for everyone.
Outbreaks in long-term care facilities have driven the high fatality rates among older adults

Our perception of the risk due to age has been strongly influenced by the terrible outbreaks in long-term care (LTC) facilities like nursing homes and assisted living centers. Nearly half of confirmed COVID-19 deaths in the United States occurred in LTC facilities, including 55 percent of deaths among Americans ages 65 and older (2). Excluding New York from the calculation, the share of older adult deaths that occurred in LTC rises to 64 percent. Excluding New York is warranted because the number of deaths in LTC facilities in New York is distorted because New York—alone among all states—reports the deaths of nursing home residents as hospital deaths when they are transferred to a hospital just before death.
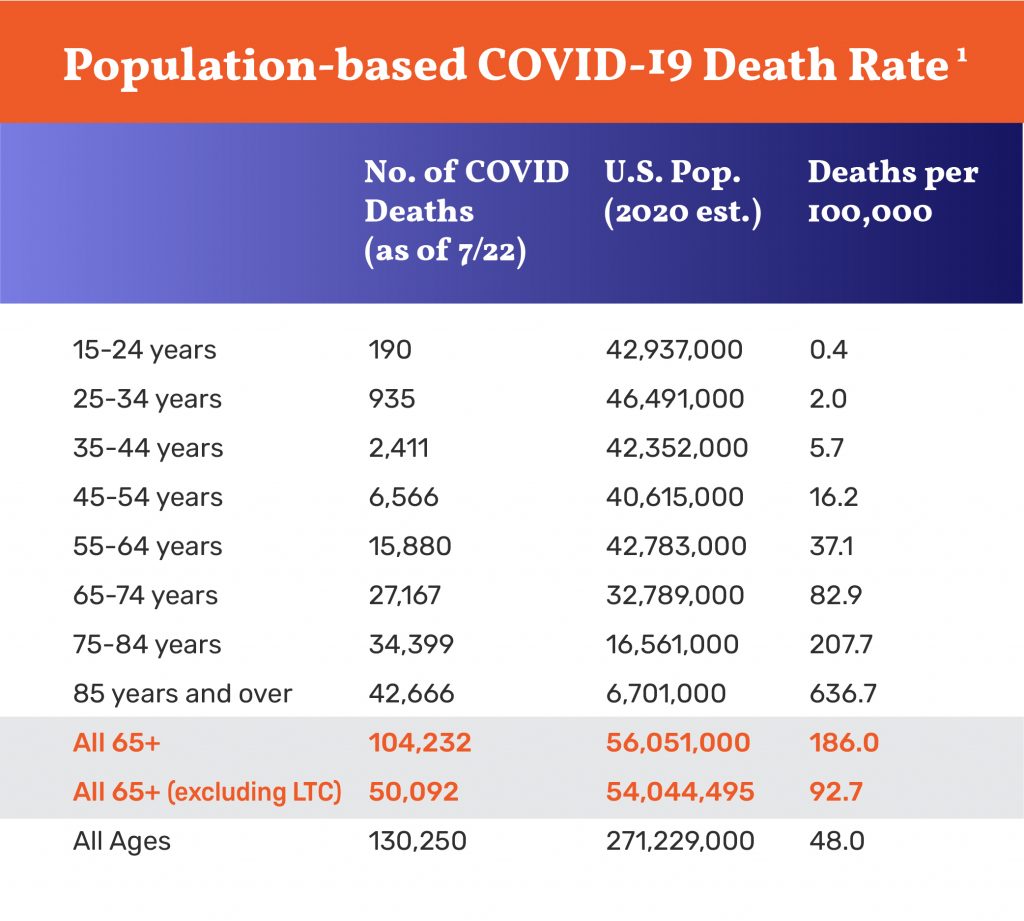
Frustratingly, it is not possible to calculate accurate death rates by age for community-dwelling older adults directly because the LTC deaths data is not disaggregated by age. For the purposes of these calculations, we assume all LTC deaths occurred among people age 65 and older since more than four out of every five LTC residents are age 65 and older (3). As shown in the table below, the huge jump in the death rate for older adults is largely driven by the LTC population. While the death rate among all Americans age 65 and above is 186 per 100,000 people, when the 54,000 long-term care facility resident deaths are removed from that figure, the death rate drops by about half.
Healthy older people under age 85 are at lower risk than many younger people with underlying conditions.
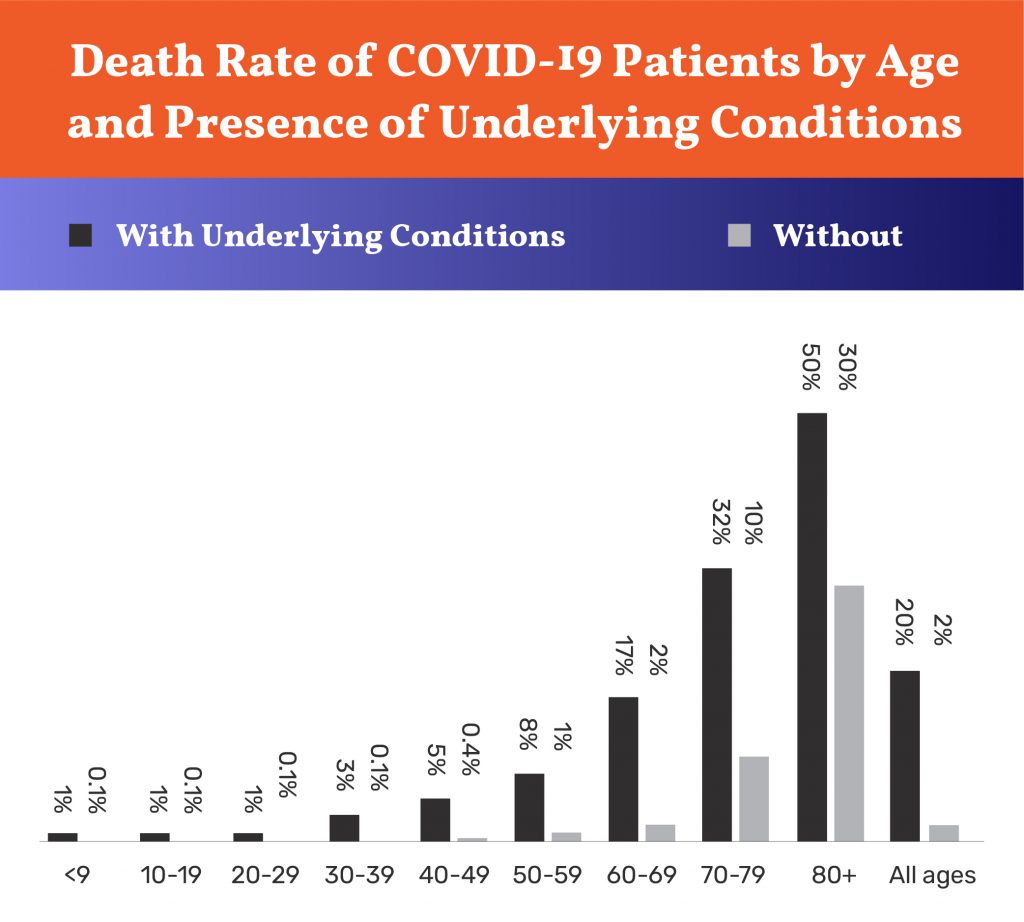
A CDC study of a sample of COVID-19 cases shows that people of any age with underlying conditions are at roughly double the risk of serious illness or death if infected. The death rate of people of any age without underlying conditions is 2 percent, compared to a death rate of people with underlying conditions of 20 percent (4). When data on underlying conditions is crossed with age data, it shows that younger people with underlying conditions are at greater risk than many healthy older people.
The CDC currently recognizes that the risk of death from COVID-19 is higher for people with a wide range of underlying conditions, including cancer, chronic kidney disease, chronic obstructive pulmonary disease (COPD), obesity, heart disease, diabetes, and others. Some evidence points to increased risk among people with asthma, high blood pressure, smokers, and even pregnant women (5).
As the table below shows, while the very oldest are at the highest risk of death (and of living in LTC facilities), many younger people with underlying conditions are at greater risk than healthy older people. Notably, the death rate for healthy people ages 60-69—the age of the majority of older workers—is about the same as the average for all ages, 2 percent. The death rate for healthy 70 to 79 year-olds is half that of people of all ages with underlying conditions. For healthy people ages 50-59 the rate is lower than the population average. Clearly, age alone is a poor predictor of the risk of death from COVID-19.
Shoddy data collection obscures the patterns that matter
That policymakers have missed these patterns is not surprising. Data on COVID-19 case outcomes is shockingly inconsistent from state to state. Most states report the age of most COVID-19 patients, but only a handful of states publicly report outcomes for long-term care residents. And New York—the state that is home to more than one out of every five Americans who have died of COVID-19 so far—reports many of the deaths of long-term care residents as hospital deaths, thus further skewing the national numbers.

Collecting data on underlying conditions is also complicated. Doing so is only possible by painstakingly going through the medical records of each case to look for red flags in their medical history. This is how the CDC was able to do their research, which is based on a subset of cases that they were able to track down in this way. The underlying conditions data is further complicated by the fact that many people with underlying conditions may not have accurate and accessible medical records. Diagnosis and treatment of these conditions depend significantly on access to adequate health care services and thus vary by race, ethnicity, age, and geography. Thus, the CDC estimates almost certainly represent an undercount of the effect of underlying conditions on the nation’s COVID-19 death toll.
Under a normal administration in the White House, the CDC would have had the authority to direct all states to collect comprehensive data on all COVID-19 cases. Robust, consistent data collection would have allowed public health authorities to see critical patterns in the case data more quickly. Instead, researchers like us are depending on a patchwork of data from different sources to figure out what is really going on. The Trump Administration’s recent decision to revoke data collection responsibility from the CDC and place it more directly under White House control will likely exacerbate this situation.
Conclusion and Recommendations
To answer the question about whether eliminating specific groups of workers will allow us to safely return to in-person work more quickly, consider the evidence: a large portion of the deaths due to COVID-19 (about 45 percent) are in long-term care facilities. An estimated 55 to 65 percent of deaths among people age 65 and above are in LTC facilities. Though the preponderance of deaths among older adults has established age as a primary driver of risk, further analysis shows that specific underlying conditions have an even stronger influence on death rates than age. Crucially, in the 60-69 age range where most older workers fall, the risk is driven principally by the presence of underlying health conditions. And many employees (and most employers) do not know who has any of these underlying conditions and who does not.
For adults age 60-69, where most older workers fall, the risk is driven principally by underlying health conditions, not age.
Taken together, this evidence suggests that the strategy for the creation of a safer in-person workplace is to adopt both environmental and individual precautions to reduce exposure and infection for all workers, rather than isolate categories of workers based on their individual characteristics.

Obviously, the individual precautions currently recommended to guide daily life apply in the workplace: maintain physical distance whenever possible, use masks or other personal protective equipment appropriate to the situation, and regularly wash or sanitize hands.
However, as with all occupational safety and health conditions, the first strategy for prevention is environmental and work process design. These draw on lessons from other aerosolized risks and include upgrading building ventilation systems; increasing distance and decreasing density; employing physical barriers; and redesigning informal interactions in common areas like locker rooms, break rooms, cafeterias, and entryways. Workers who can do all or part of their work from home should continue to have the option to do so.
How these general strategies are executed in practice will vary by occupation and industry and largely vary by the degree of contact that workers have with each other and with the general public. For instance, congregate settings like schools, senior centers, and gymnasiums will have to undertake significant and complex mitigation strategies to protect their workers and the people they serve. Hospitals, clinics, and other medical facilities are especially critical in this regard. Manufacturing facilities may need to restructure their physical plant to optimize workflow while allowing workers to remain at a safe distance. Retail establishments may install barriers or limit the number of customers who are allowed to enter enclosed spaces in order to create a safe environment.
All workplaces must adopt environmental and individual health and safety precautions, rather than isolating categories of workers.
Making workplaces safer for every worker may seem like a big undertaking, but measures to minimize risk have been rolled out before. Though using protective gloves while handling patients has been an established practice since at least the 1890s, many medical professionals were still not using them for fear of alienating their patients. However, the HIV/AIDS pandemic ushered in the adoption of “universal precautions” by all health workers, increasing usage. While that was a difficult task then, today the thought of a dentist or phlebotomist not wearing gloves would be bizarre. We can solve the occupational health puzzle, but only if we ask the right questions.
Notes
[1] Total COVID deaths data from CDC, Provisional COVID-19 Death Counts by Sex, Age, and State. Accessed at https://data.cdc.gov/NCHS/Provisional-COVID-19-Death-Counts-by-Sex-Age-and-S/9bhg-hcku. Population estimates from U.S. Census, 2017 National Population Projections Tables: Main Series. Table 3. Detailed age and sex composition of the population. Accessed at https://www.census.gov/data/tables/2017/demo/popproj/2017-summary-tables.html. Estimated COVID deaths in long-term care facilities from Girvan, Gregg, and Avik Roy (updated July 14, 2020), “Nursing Homes & Assisted Living Facilities Account for 45% of COVID-19 Deaths,” The Foundation for Research on Equal Opportunity (FREOPP). Accessed at https://freopp.org/the-covid-19-nursing-home-crisis-by-the-numbers-3a47433c3f70.
[2] Share of COVID-19 deaths among older adults are from author’s calculations based on data from the state health departments of each reporting state. Share of COVID-19 deaths that occurred among residents of long-term care facilities is from Girvan and Roy (see note 1 above). This estimate is based on imperfect data. Not all states report deaths in long-term care facilities and those that do report do not do so regularly. Also, a few states do not report disaggregated data by age.
[3] National Center for Health Statistics. Vital and Health Statistics Series 3, Number 43, February 2019. Accessed at https://www.cdc.gov/nchs/data/series/sr_03/sr03_43-508.pdf.
[4] CDC. (2020, June). “People Who Are at Increased Risk for Severe Illness.” Accessed at https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-at-increased-risk.html.
[5] CDC (2020, July). People with Certain Medical Conditions. https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html
